by Lindsey Valich
Explorers have dreamt for centuries of a Fountain of Youth, with healing waters that rejuvenate the old and extend life indefinitely.
Researchers at the University of Rochester, however, have uncovered more evidence that the key to longevity resides instead in a gene.
In a new paper published in the journal Cell, the researchers—including Vera Gorbunova and Andrei Seluanov, professors of biology; Dirk Bohmann, professor of biomedical genetics; and their team of students and postdoctoral researchers—found that the gene sirtuin 6 (SIRT6) is responsible for more efficient DNA repair in species with longer lifespans. The research illuminates new targets for anti-aging interventions and could help prevent age-related diseases.
Inevitable double-strand breaks
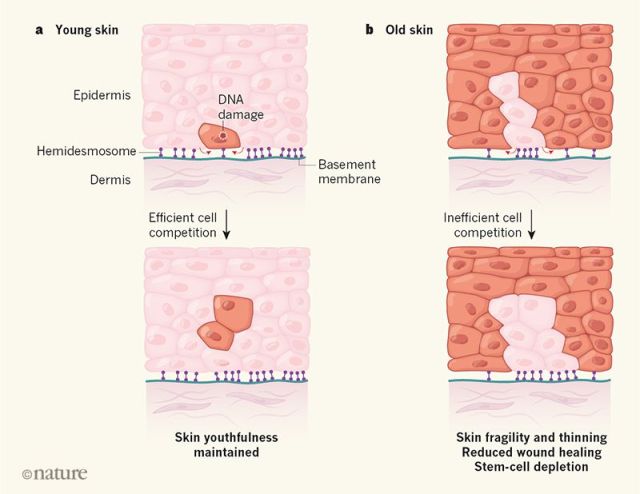
As humans and other mammals grow older, their DNA is increasingly prone to breaks, which can lead to gene rearrangements and mutations—hallmarks of cancer and aging. For that reason, researchers have long hypothesized that DNA repair plays an important role in determining an organism’s lifespan. While behaviors like smoking can exacerbate double-strand breaks (DSBs) in DNA, the breaks themselves are unavoidable. “They are always going to be there, even if you’re super healthy,” says Bohmann. “One of the main causes of DSBs is oxidative damage and, since we need oxygen to breathe, the breaks are inevitable.”
Organisms like mice have a smaller chance of accumulating double-strand breaks in their comparatively short lives, versus organisms with longer lifespans, Bohmann says. “But, if you want to live for 50 years or so, there’s more of a need to put a system into place to fix these breaks.”
The longevity gene
SIRT6 is often called the “longevity gene” because of its important role in organizing proteins and recruiting enzymes that repair broken DNA; additionally, mice without the gene age prematurely, while mice with extra copies live longer. The researchers hypothesized that if more efficient DNA repair is required for a longer lifespan, organisms with longer lifespans may have evolved more efficient DNA repair regulators. Is SIRT6 activity therefore enhanced in longer-lived species?
To test this theory, the researchers analyzed DNA repair in 18 rodent species with lifespans ranging from 3 years (mice) to 32 years (naked mole rats and beavers). They found that the rodents with longer lifespans also experience more efficient DNA repair because the products of their SIRT6 genes—the SIRT6 proteins—are more potent. That is, SIRT6 is not the same in every species. Instead, the gene has co-evolved with longevity, becoming more efficient so that species with a stronger SIRT6 live longer. “The SIRT6 protein seems to be the dominant determinant of lifespan,” Bohmann says. “We show that at the cell level, the DNA repair works better, and at the organism level, there is an extended lifespan.”
The researchers then analyzed the molecular differences between the weaker SIRT6 protein found in mice versus the stronger SIRT6 found in beavers. They identified five amino acids responsible for making the stronger SIRT6 protein “more active in repairing DNA and better at enzyme functions,” Gorbunova says. When the researchers inserted beaver and mouse SIRT6 into human cells, the beaver SIRT6 better reduced stress-induced DNA damage compared to when researchers inserted the mouse SIRT6. The beaver SIRT6 also better increased the lifespan of fruit flies versus fruit flies with mouse SIRT6.
Species with even more robust SIRT6?
Although it appears that human SIRT6 is already optimized to function, “we have other species that are even longer lived than humans,” Seluanov says. Next steps in the research involve analyzing whether species that have longer lifespans than humans—like the bowhead whale, which can live more than 200 years—have evolved even more robust SIRT6 genes.
The ultimate goal is to prevent age-related diseases in humans, Gorbunova says. “If diseases happen because of DNA that becomes disorganized with age, we can use research like this to target interventions that can delay cancer and other degenerative diseases.”
https://phys.org/news/2019-04-longevity-gene-responsible-efficient-dna.html